May 11 2020
Likely No Summer Break from COVID-19
 As is often pointed out, the SARS-CoV2 virus is new, and therefore we have limited data on its characteristics, as well as the disease it causes, COVID-19. This complicates our modeling of what is likely to happen, and recommendations about best practices. But scientists around the world are busy studying this pandemic as it is occurring, and therefore our models and recommendations are evolving.
As is often pointed out, the SARS-CoV2 virus is new, and therefore we have limited data on its characteristics, as well as the disease it causes, COVID-19. This complicates our modeling of what is likely to happen, and recommendations about best practices. But scientists around the world are busy studying this pandemic as it is occurring, and therefore our models and recommendations are evolving.
Already we know quite a bit. For example, one review of NYC patients found:
Among the 393 patients, the median age was 62.2 years, 60.6% were male, and 35.8% had obesity. The most common presenting symptoms were cough (79.4%), fever (77.1%), dyspnea (56.5%), myalgias (23.8%), diarrhea (23.7%), and nausea and vomiting (19.1%). Most of the patients (90.0%) had lymphopenia, 27% had thrombocytopenia, and many had elevated liver-function values and inflammatory markers. Between March 3 and April 10, respiratory failure leading to invasive mechanical ventilation developed in 130 patients (33.1%); to date, only 43 of these patients (33.1%) have been extubated. In total, 40 of the patients (10.2%) have died, and 260 (66.2%) have been discharged from the hospital; outcome data are incomplete for the remaining 93 patients (23.7%).
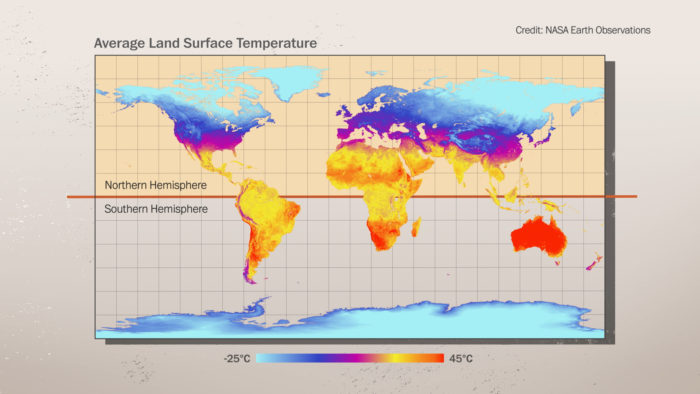
One question, which is especially important as the northern hemisphere approaches summer, is if SARS-CoV2 is less virulent in warmer temperatures. Coronaviruses in general tend to spread less in warmer months, so there is some reason to hope this will be the case. However, a new review of COVID-19 data pokes a hole in this hope. The authors looked at many countries around the world and correlated the number of new cases with various factors, including temperature and humidity.
To estimate epidemic growth, researchers compared the number of cases on March 27 with cases on March 20, 2020, and determined the influence of latitude, temperature, humidity, school closures, restrictions of mass gatherings and social distancing measured during the exposure period of March 7 to 13.
They found no correlation between the number of cases and temperature, and only a weak association of reduced spread with increased humidity. This is, perhaps, the most comprehensive study to date. There have been numerous previous studies, mostly regional, that do show a negative correlation with virus spread and temperature. The authors suggest this is due partly to lack of rigor in those studies. Also, an expert review of this data (prior to the most recent study) urged caution. They note that the studies showed inconsistent results, and it is difficult to generalize the data to what is likely to happen in the world with COVID-19.
There are basically two factors to consider here. The first is the inherent activity of the virus itself, and to what extent it is affected by temperature and humidity. It is likely that, as with most organisms, there is an ideal temperature range for this virus, and too warm or too cold conditions will limit its ability to thrive. However, it may do just fine in the range of temperatures in which humans live. The second factor, however, is the nature of pandemics themselves. It may be true that the virus is so virulent and contagious (as we would expect for a virus capable of causing a pandemic) that small changes in virulence due to temperature are simply not that meaningful. Also, the fact that this is a novel virus and the world’s population is immunologically naive to it may simply be a superseding factor. The expert review reports:
They added that neither the coronaviruses that cause severe acute respiratory syndrome (SARS) and Middle East respiratory syndrome (MERS) nor the flu strains of previous pandemics have shown a seasonal pattern.
“There have been 10 influenza pandemics in the past 250-plus years—two started in the northern hemisphere winter, three in the spring, two in the summer and three in the fall,” they said. “All had a peak second wave approximately six months after emergence of the virus in the human population, regardless of when the initial introduction occurred.”
So if looking at how pandemics of respiratory illnesses behave, they are not seasonal, and they tend to have a second wave six months after the original wave (regardless of season). This may have to do more with the dynamics of pandemics than the details of each specific virus. Given all this the experts warn that we cannot expect the summer to save us from this pandemic, and we should be prepared for a second wave in the Fall.
But there is some good news in the data of this recent study as well:
The researchers did find that public health measures, including school closures, social distancing and restrictions of large gatherings, have been effective.
It’s good to have some empirical confirmation that the measures of social distancing we are taking are actually working. This is important information to get to the public who are making incredible sacrifices on the hope that it will “flatten the curve,” prevent our health care systems from getting overwhelmed, and save lives. Well, it is. This is especially important as we are beginning to relax social distancing.
All data regarding COVID-19 should be considered preliminary and subject to further research. But still, we need to act now with the best scientific information we have now. This includes the risks and benefits of everything we do, and everything we don’t do. Several years from now when we are able to look back at the pandemic with some perspective, we will be able to see how it all worked out. Until then we are trying to view this storm from within it. Still it is amazing how many scientific studies are coming out – we have a flood of data, and this is helping guide us through the storm.






