Nov 13 2012
Communicating with the Vegetative
A BBC program, Panorama, will soon air a show in which they explore a new technique for communicating with people who were believed to be in a vegetative state. The technique is based on research published in 2010 in the NEJM: Willful Modulation of Brain Activity in Disorders of Consciousness.
This is an intriguing area of research that I have been following and writing about here for the past few years. For background, vegetative patients are those who have suffered a brain injury of some sort and are no longer able to display any outward sign of consciousness. They tend to go through sleep-wake cycles, they open their eyes and have roving eye movements, but there is no indication on exam of purposeful activity or any objective response to their environment (this is by definition). If such patients show some signs of consciousness or response to external stimuli then they are deemed to be in a minimally conscious state.
One challenge is that such patients are unable to communicate directly. We have to infer their consciousness (or lack thereof) from the neurological exam. Even an enhanced exam designed to look for subtle signs of consciousness is still a crude instrument. We have no way of directly looking at the “mind” of the patient to see what their experience of consciousness is. There is some utility to such exams, however. In one study 40% of patients thought to be in a persistent vegetative state by routine evaluation were found to be in a minimally conscious state by a more elaborate neurological exam.
Recent studies have also shown that if EEG or fMRI techniques are used to assess brain activity in patients thought to be vegetative, some show signs that they may in fact be minimally conscious. The difference is subtle but may be meaningful. In terms of prognosis, there is a tiny but non-zero difference. Patients who are truly persistent vegetative essentially have no chance of meaningful recovery, while patients in a minimally conscious state have a very small chance of some recovery – meaning they may be able to wake up to the point that they can attend to people in their environment and participate in their care, such as feeding. In no case has someone in such a state for years awakened to anything near normal neurological function. (Short term comas are a different story – in this article I am talking about long term chronic conditions).
One possible difference for the future is response to new experimental treatments, such as implanting computer chips to augment brain function and allow for improved neurological function. This is more likely to work in those who are minimally conscious than those who are truly vegetative.
Finally, if a patient in a coma has a flicker of consciousness then perhaps it may be possible to communicate with them. They cannot move or speak to communicate their thoughts, but those thoughts are there, trapped inside their brain. The NEJM study uses functional MRI scanning to look at blood flow to different parts of the brain as a way of inferring brain activity. In the study the researchers ask patients to imagine themselves either playing tennis (which should activate the premotor area) and walking through their home (which should activate the visuospatial area). In healthy control subjects the two mental tasks result in distinct fMRI patterns.
The study tested the technique on 54 patients in a persistent vegetative or minimally conscious state. In 5 of the 54 subjects, they were able to reproducibly demonstrate the target fMRI pattern in response to the task given (imagining playing tennis or walking around their home). If these results are correct that would be a significant sign of some consciousness. At the very least this would be a more sensitive test to detect patients who are in a minimally conscious state.
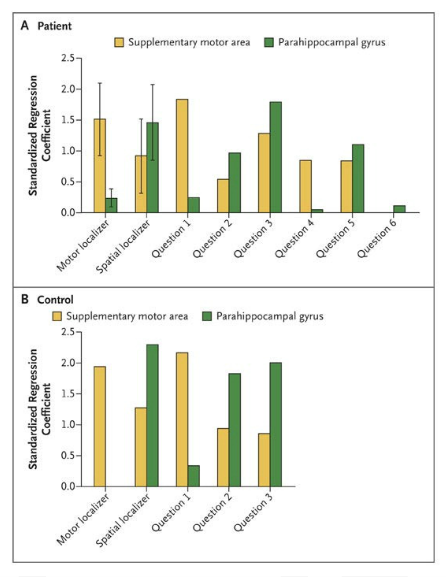 There are reasons for skepticism regarding such results, although the researchers believe they are robust. First, fMRI scanning is a tricky technique that requires careful procedures to avoid overinterpreting random brain activity. Look at the graph – the error bars on the regional activity are fairly large. While statistically the results seem valid, the large amount of noise in the results is always cause for caution.
There are reasons for skepticism regarding such results, although the researchers believe they are robust. First, fMRI scanning is a tricky technique that requires careful procedures to avoid overinterpreting random brain activity. Look at the graph – the error bars on the regional activity are fairly large. While statistically the results seem valid, the large amount of noise in the results is always cause for caution.
One factor that causes me to be more likely to accept the results as real is that all 5 of the subjects who responded were in their state due to traumatic injury. Prior research shows that subjects in a coma from trauma are more likely to have greater cognitive function than their exam may indicate. Meanwhile patient who are vegetative because of a diffuse anoxic ischemic injury generally do not.
The reason for this is that patients in a vegetative state from lack of oxygen to the whole brain have fairly uniform damage to their whole brain. It makes sense that if they appear vegetative it is because they are. Patients who have suffered physical trauma, like a car accident, however, have variable damage to different parts of their brain, so it is possible that some parts of the brain are working relatively fine while others are severely damaged. This latter scenario is more likely to result in a situation where a patient has some consciousness but is physically unable to speak or move, and so has hidden consciousness.
I therefore find it telling that all 5 of the 54 test subjects were those with traumatic injury, rather than anoxia or a similarly diffuse cause of their vegetative state.
My sense of the data overall is that it is fairly robust, and it is plausible, but I would still like to see some further replications to make sure that the results are not just an illusory pattern pulled out of the noise.
Another caution I have is in the interpretation of the results. It may be that some patients in a minimally conscious state are able to respond to verbal commands, but still may have limited or no awareness. We just don’t know how they are experiencing the exchange, if at all. We do not yet understand enough about the neuroanatomical correlates of consciousness to predict the net function in a brain with patchy damage to various areas.
Assuming the results are real – what does this mean. First, it supports prior research that indicates that some patients who appear vegetative on exam are actually in a minimally conscious state. This study takes it one step further, however, and shows that using fMRI it is possible to communicate with a small minority of such patients, to get basic yes or no answers from them. This could be used to direct their care and perhaps improve their quality of life.
The technology may also be helpful from a purely diagnostic point of view. For 49 of the studied patients they were unable to consciously modulate their brain activity in response to questions. This gives us greater confidence in the diagnosis of persistent vegetative state in these individuals and is reassuring that we are not missing hidden cognitive function because of the limitation of the neurological exam. Sometimes families and doctors may differ in their assessment of the function of an injured loved-one. Families may believe, for example, that occasional movement or eye contact on the part of a patient indicates some awareness, while health care staff may be more conservative in interpreting such evidence. A more definitely negative fMRI study, however, could be helpful in convincing the family that there truly is no awareness and this may further help with decisions about aggressiveness of care.
And of course for the small number of patients who exhibit awareness on the fMRI test this would also inform aggressiveness of treatment, and may also be used to help direct care.
While still preliminary, this is exciting research. It will become increasingly more exciting not only as the technology and techniques are refined, but as new potential treatments for the brain injured come closer to reality. The two big areas where I see potential are in stem cell treatments and brain-machine interfaces. We still cannot predict if these technologies will pan out anytime soon, but they are plausible and exciting possibilities.






