Sep 21 2023
Immune Cells to Fight Cancer
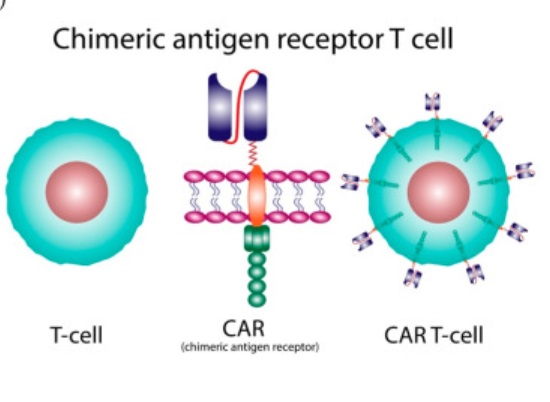 There is a recent medical advance that you may not have heard about unless you are a healthcare professional or encountered it from the patient side – CAR-T cell therapy. A recent study shows the potential for continued incremental advance of this technology, but already it is a powerful treatment.
There is a recent medical advance that you may not have heard about unless you are a healthcare professional or encountered it from the patient side – CAR-T cell therapy. A recent study shows the potential for continued incremental advance of this technology, but already it is a powerful treatment.
Like all technologies, the roots go back pretty far. It was first discovered that immune cells protect against cancer in 1960. In 1986 tumor-infiltrating lymphocytes were used to attack cancer cells. In 1993 the first generation of genetically modified T-cells using the chimeric antigen receptor (CAR) technique was developed. This technique fuses the business end of an antibody to a receptor on a T-cell (hence a chimera) which potentially targets that T-cell against whatever antigen the antibody targets. So you can make antibodies against a protein unique to a specific type of cancer, then fuse part of that antibody to T-cell receptors, put those T-cells back into the patient and they will potentially attack the cancer cells. This first generation CAR-T cells were not effective clinically because they did not survive long enough in the body to work.
In 1998 it was discovered that adding a costimulatory domain (CD28) to the CAR allowed it to persist longer in the body, creating the potential for clinical treatment. In 2002 this technique was used to develop second generation CAR-T cells that were shown for the first time to fight cancer in mice (the first study was of prostate cancer). Then in 2003 CAR-T cells using CD19 instead of CD28 were developed, and found to be more effective. In 2013 the first clinical trial in humans showing efficacy of CAR-T therapy in cancer (leukemia) was published, starting the era of using CAR-T therapy in treating blood cancers. The first CAR-T base treatment was approved by the FDA in 2017.
Over the last 8 years CAR-T therapy has become standard treatment for blood-born cancers (lymphoma and acute lymphoblastic leukemia). T-cells are taken from patients with cancer, they are then genetically modified into CAR-T cells, reproduced to make lots of them, and then given back to the patient to fight their cancer. In the last decade scientific advance has continued, with research targeting other proteins to potentially fight solid tumors. In 2017 scientists starting using CRISPR technology to make their CAR-T cells allowing greater control and improved function.

 Japan is planning on releasing treated radioactive water from the Fukushima nuclear accident into the ocean. They claim this will be completely safe, but there are
Japan is planning on releasing treated radioactive water from the Fukushima nuclear accident into the ocean. They claim this will be completely safe, but there are 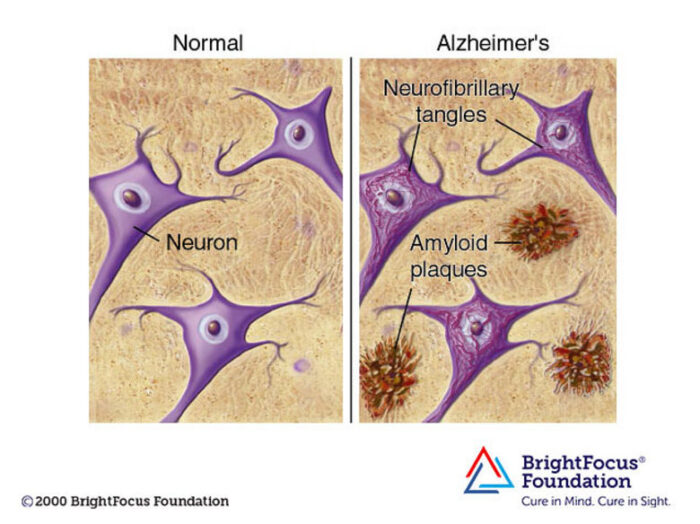 Decades of complex research and persevering through repeated disappointment appears to be finally paying off for the diagnosis and treatment of Alzheimer’s disease (AD). In 2021 Aduhelm was the first drug approved by the FDA (granted contingent accelerated approval) that is potentially disease-modifying in AD. This year
Decades of complex research and persevering through repeated disappointment appears to be finally paying off for the diagnosis and treatment of Alzheimer’s disease (AD). In 2021 Aduhelm was the first drug approved by the FDA (granted contingent accelerated approval) that is potentially disease-modifying in AD. This year Despite robust efforts to fight it, malaria remains one of the most significant infectious diseases affecting humans.
Despite robust efforts to fight it, malaria remains one of the most significant infectious diseases affecting humans. 
 Some ideas never seem to die. There is something compelling about the narrative, perhaps because it fills some explanatory need. One of those narratives is that “they” have “the cure” to cancer but are keeping it hidden from the public in order to protect the profits that result from cancer treatment. I recently received the following e-mail (partly redacted):
Some ideas never seem to die. There is something compelling about the narrative, perhaps because it fills some explanatory need. One of those narratives is that “they” have “the cure” to cancer but are keeping it hidden from the public in order to protect the profits that result from cancer treatment. I recently received the following e-mail (partly redacted):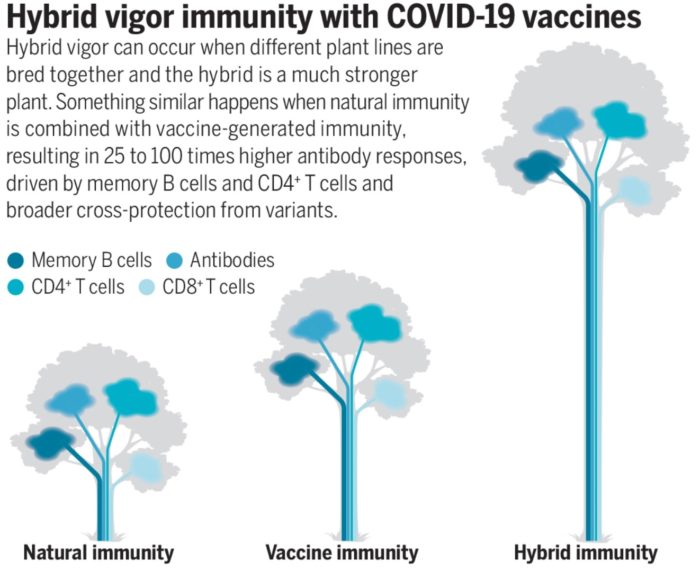 As many experts predicted, the COVID-19 pandemic is slowly sliding into an endemic infection. A pandemic is essentially when an epidemic goes worldwide. Endemic means that an infection is here to stay. It is no longer considered an “outbreak” but is constantly spreading around a population without having to be introduced. The flu, for example, is endemic, although it is also seasonal. Measles was endemic in the US, but then was eliminated through vaccination and was reduced to isolated outbreaks. However, it is transitioning to being endemic again because of vaccine hesitancy.
As many experts predicted, the COVID-19 pandemic is slowly sliding into an endemic infection. A pandemic is essentially when an epidemic goes worldwide. Endemic means that an infection is here to stay. It is no longer considered an “outbreak” but is constantly spreading around a population without having to be introduced. The flu, for example, is endemic, although it is also seasonal. Measles was endemic in the US, but then was eliminated through vaccination and was reduced to isolated outbreaks. However, it is transitioning to being endemic again because of vaccine hesitancy.




