Jan 21 2020
Immunology Cancer Discovery
 The BBC headline reads: Immune discovery ‘may treat all cancer’. Most health headlines, even of legitimate scientific discoveries, tend to be overhyped. All health discoveries, apparently, will either eventually cure cancer or the common cold. This headline is also overhyped, in my opinion, but this is a legitimate discovery with possible implications for future cancer treatment.
The BBC headline reads: Immune discovery ‘may treat all cancer’. Most health headlines, even of legitimate scientific discoveries, tend to be overhyped. All health discoveries, apparently, will either eventually cure cancer or the common cold. This headline is also overhyped, in my opinion, but this is a legitimate discovery with possible implications for future cancer treatment.
What the scientists discovered was an immune receptor which seems to target most cancer cells while not targeting healthy cells. This certainly seems like the kind of thing that can potentially be exploited in immune therapy for cancer. The actual title of the study is: Genome-wide CRISPR–Cas9 screening reveals ubiquitous T cell cancer targeting via the monomorphic MHC class I-related protein MR1.
The CRISPR angle is interesting, and not mentioned in the BBC article. It is another example of how CRISPR is turbocharging genetics research. The researchers used it to comb the genome and they found a receptor found on T-cells, the MR1, that seems to target all cancer cells but not non-cancer cells. Further, the targeting seems to be via the cancer cell metabolism. Somehow the receptor is sensing the altered metabolism of the cancer cells. Importantly, it is targeting a feature of that metabolism that is common to most if not all types of cancer:
“The Cardiff team discovered a T-cell and its receptor that could find and kill a wide range of cancerous cells in the lab including lung, skin, blood, colon, breast, bone, prostate, ovarian, kidney and cervical cancer cells.”
This is the point where I need to emphasize that this is basic science research, not clinical research. It is also very early research, which means it has opened up a long list of further research questions that need to be answered. I have been in the field long enough to develop a sense of where research is in the arch of progress from basic science to the clinic. The immunotherapies for cancer that have been coming out in the past few years I first heard about in the 1990s. A 20-30 year delay from when basic science research first suggests a possible treatment, to treatments being approved for clinical use, is typical. The pace may be increasing a bit because of the technology of basic science research. CRISPR is an excellent example of this. But clinical research just takes time. It needs to progress from animal research through multiple stages of human research, even for a single indication. Then subsequent research is necessary to further understand how the treatment works for which diseases and which patients.
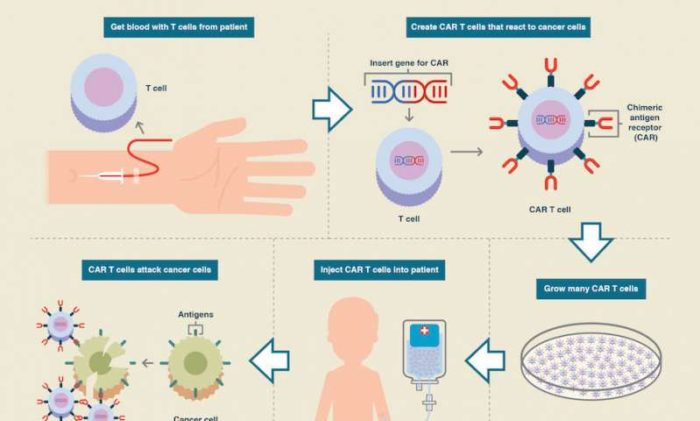
The good news for this new finding is that the basic technology is already in use – immunotherapy for cancer. So we are, in essence, already half-way there. So maybe 10-15 years is more optimistic, if everything goes well. There are actually several types of cancer immunotherapy, which involved enhancing or targeting the immune system in some way to better fight off cancer. The one most relevant to this new discovery is called CAR (chimeric antigen receptors) T-cell therapy. This type of cancer immunotherapy involves taking blood from a patient with cancer and then filtering out their T-cells. A virus is then used to insert a gene into the T-cells providing a receptor which targets the patient’s specific cancer type. For example, the CD19 receptor is used to target leukemia and lymphoma, types of blood-born cancer. Different receptors would be needed to target other cancers.
So the breakthrough here is that the researchers found a receptor which seems to be ubiquitous to all cancer types – at least all of those tested. So theoretically we can use the CAR T-cell approach, but use the MR1 receptor instead of a cancer-specific receptor. Of course, you can also do both for hopefully additive effect. But the CAR T MR1 therapy could theoretically treat any cancer type.
But there is still one major fly in this ointment – the CAR T-cell therapy is very effective at treating blood-born cancers, not so much solid tumors. This is probably a practical effect of the CAR T-cells gaining access to the cancer cells, but there may be other obstacles as well. This is currently an area of active research. So this is a distinct problem that may need to be solved in order for CAR T therapy with MR1 to become a truly universal cancer treatment.
Again, if history is any guide, what typically has happened is that a new cancer treatment sounds like a cure for cancer when first introduced, and then ultimately becomes an important additional treatment in the oncology armamentarium, but it is just one cumulative small step forward. I have little doubt this new discovery will add to our cancer-treating technology. It does seem very promising, and fits nicely into an established therapy. The question is, how effective will it be, and how truly universal will be its applicability?
Of course I hope this will be the one breakthrough that will truly cure all cancer, but history suggests caution. Realistically, I hope this will turn out to be a somewhat larger step forward.






