Oct 20 2011
Malaria Vaccine
Malaria is a serious illness in humans caused by several species of mosquito-born parasite (Plasmodium falciparum, vivax, and ovale). The CDC reports:
In 2008, an estimated 190 – 311 million cases of malaria occurred worldwide and 708,000 – 1,003,000 people died, most of them young children in sub-Saharan Africa.
Efforts to reduce the incidence of malaria have largely focused on reducing the number of mosquitoes and preventing bites (for example by providing netting to cover beds), and these efforts can be very successful. But despite these measures malaria remains the 5th largest cause of death worldwide from infectious disease.
It was therefore exciting news when GlaxoSmithKline (GSK) announced a successful clinical trial of a new anti-malaria vaccine. The vaccine is the result of 24 years of research led by Joe Cohen. The report:
Final stage clinical trial data on RTS,S, also known as Mosquirix, showed it halved the risk of African children getting malaria, making it likely to become the world’s first successful vaccine against the deadly disease.
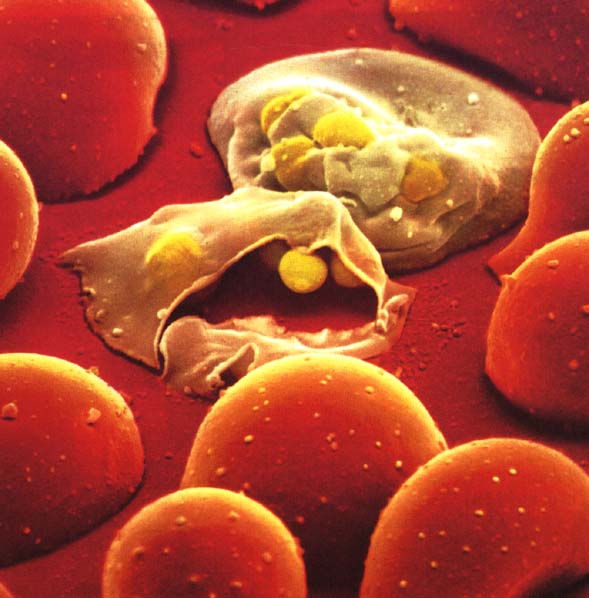 The vaccine is targeted at the liver stage of the parasite, keeping it from multiplying and giving the body a chance to wipe it out before it returns to the blood. In a clinical trial of 16,000 children, the largest clinical trial ever conducted in Africa, the vaccine proved to be safe and about 50% effective. That leaves a lot of room for improvement. Clearly this one vaccine by itself will not be enough to eradicate malaria, but it can significantly reduce the burden of this disease. Further research will hopefully improve its efficacy over time.
The vaccine is targeted at the liver stage of the parasite, keeping it from multiplying and giving the body a chance to wipe it out before it returns to the blood. In a clinical trial of 16,000 children, the largest clinical trial ever conducted in Africa, the vaccine proved to be safe and about 50% effective. That leaves a lot of room for improvement. Clearly this one vaccine by itself will not be enough to eradicate malaria, but it can significantly reduce the burden of this disease. Further research will hopefully improve its efficacy over time.
GSK estimates that if all goes well they should be able to have the vaccine on the market by 2015. Let’s hope all goes well. It will be interesting to watch the effect of this vaccine on the incidence and disease burden of malaria for the decade following the start of its use. The 50% reduction might have a magnified effect due to reducing the spread of the parasite by interrupting its life cycle. This degree of protection is not enough to provide “herd immunity” but it will still help reduce the prevalence of the parasite.
Other methods of fighting malaria will still be necessary, such as reducing mosquito populations and providing protective netting. I hope the use of the vaccine does not provide a false sense of security that reduces the use of other measures. This could have a paradoxically negative effect. There are many examples of this – such as people using sunscreen getting excessive sun exposure, or people who think they are driving a safe car driving more recklessly. So use of the vaccine will need to be combined with education measures to be sure the population understands this is just one of many measures that still need to be taken.
I also wonder how effect the vaccine will have to become in order for eradication to be likely. The typical figure given is 90-95%, but that applies to organisms that spread directly from person to person. I don’t know if it applies to a parasite with the complex life cycle of Plasmodium. Also, Plasmodium has non-human reservoirs, meaning some species also infect vertebrates other than humans. So even if a highly effective vaccine were available the parasite could continue to exist in these other animals. So a human vaccine alone cannot achieve eradication.
But eradication can still be achieved if the population of Plasmodium is significant reduced by reducing human hosts, and then other measures, for example aimed at the mosquito part of the life cycle, may achieve eradication. It should be noted that the CDC achieved eradication of malaria in the US without the use of a vaccine.
In any case, the vaccine is a powerful additional tool in the fight against malaria. It will likely save millions of lives and significantly help the effort to reduce or eradicate malaria worldwide.






